Understanding Perimenopause: The Transition Phase
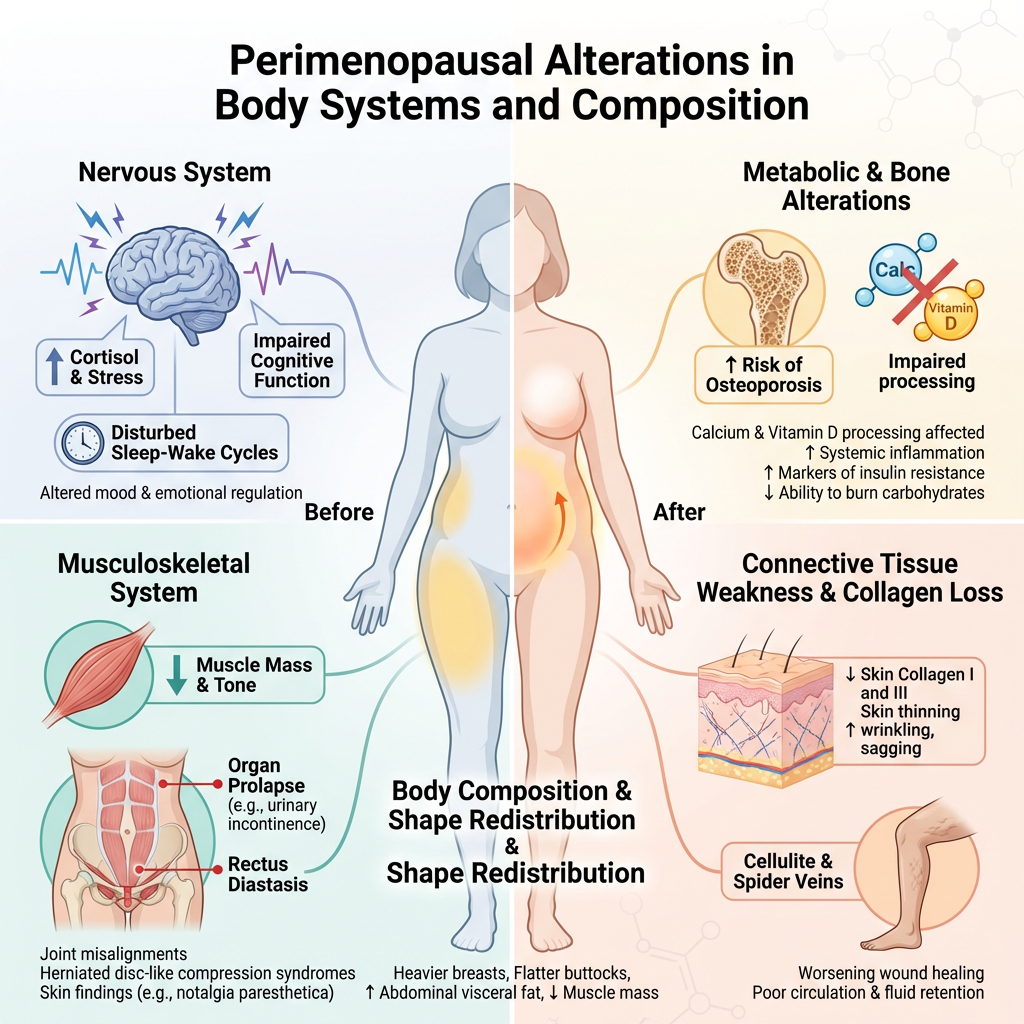
Long before menopause officially begins, your body goes through a transitional phase called perimenopause. This period can start in your 40s (or sometimes earlier) and can last anywhere from a few years to a decade. During this time, your ovaries gradually begin to produce less estrogen, leading to hormone fluctuations that can cause a surprising variety of symptoms.
At The Links Clinic in Edmonton, Dr. Sam Azer recognizes that perimenopause can be a confusing and frustrating time. You might still be getting your period, but you may not feel like yourself. Common signs include changes in your menstrual cycle (heavier, lighter, or irregular periods), mood swings, anxiety, sleep disturbances, brain fog, and the onset of hot flashes or night sweats.
How is Perimenopause Diagnosed?
There is no single definitive blood test to diagnose perimenopause, as your hormone levels naturally fluctuate day by day during this phase. Instead, Dr. Azer focuses on a comprehensive clinical evaluation. We will listen closely to your symptom history, track changes in your menstrual cycle, and rule out other potential causes for how you are feeling (such as thyroid issues). Your lived experience and symptoms are the most important diagnostic tools we use.
Tailored Treatment Options
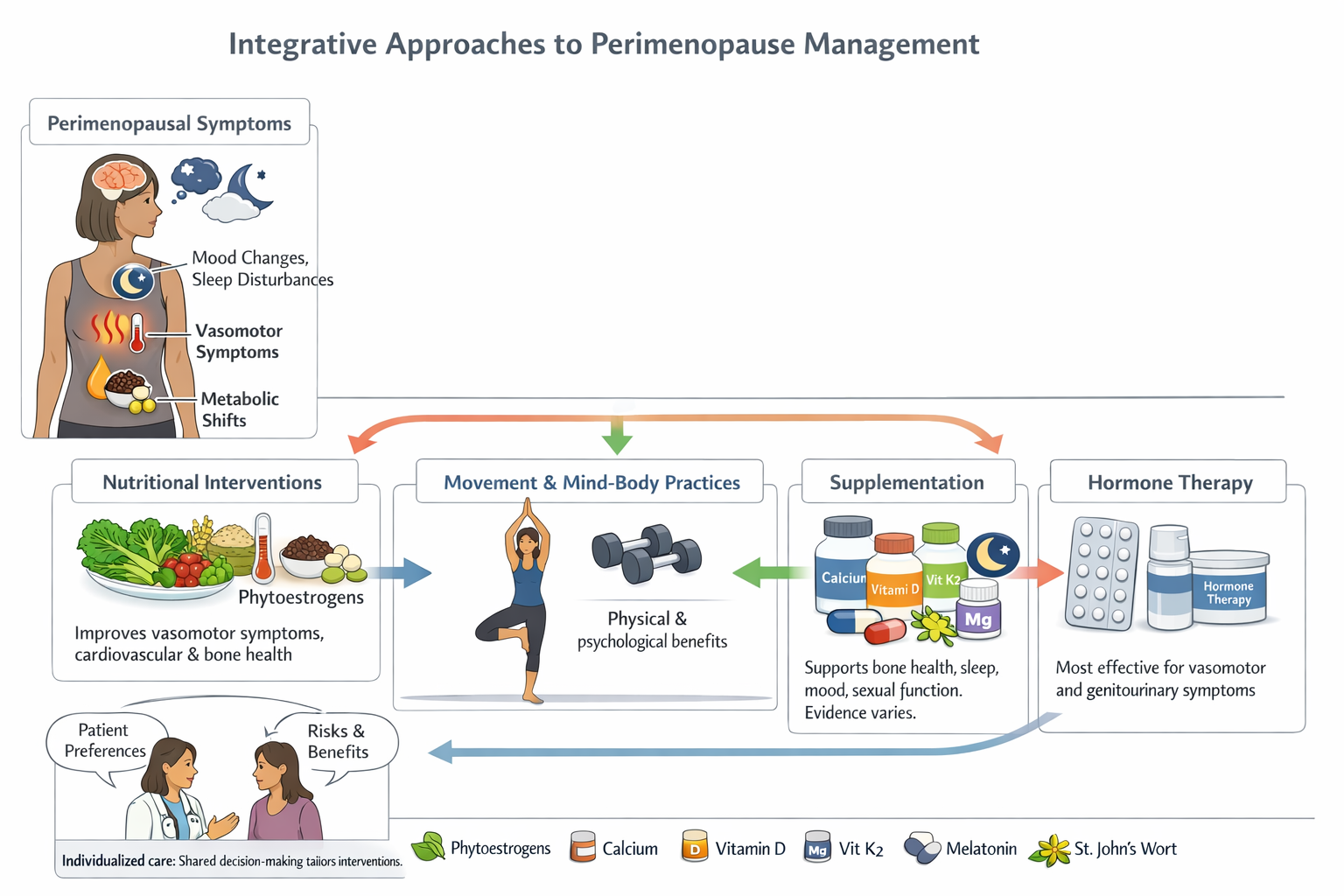
You do not have to wait until your periods stop completely to seek relief. We offer a variety of personalized options to help smooth out hormone fluctuations and manage your specific symptoms during perimenopause:
Low-Dose Hormonal Contraceptives: For many women, low-dose birth control pills or a hormonal IUD can be highly effective at regulating heavy or unpredictable periods while simultaneously relieving hot flashes and stabilizing moods.
Cyclical Hormone Therapy: Depending on your symptom severity and medical history, a carefully tailored dose of estrogen and progesterone can help bridge the gap as your natural hormone levels decline.
Non-Hormonal Medications: If hormonal options are not right for you, we can prescribe targeted, non-hormonal medications to help manage hot flashes, improve sleep quality, and support your mental well-being.
Lifestyle and Preventative Care: We will work with you to implement evidence-based lifestyle adjustments—focusing on nutrition, stress management, and bone health—to protect your long-term vitality as you move closer to menopause.